On a chilly February morning, Jassuram Khanna, a farmer from Sujau village in Chakrata in Uttarakhand, felt a tightness in his chest on his option to the market. After ready a couple of minutes, he known as his son Suresh to come back and take him to the physician. They employed a non-public automotive and went to the native Primary Health Centre (PHC), the place the well being employee checked his blood stress and despatched him to Vikasnagar, a close-by Tehsil city.
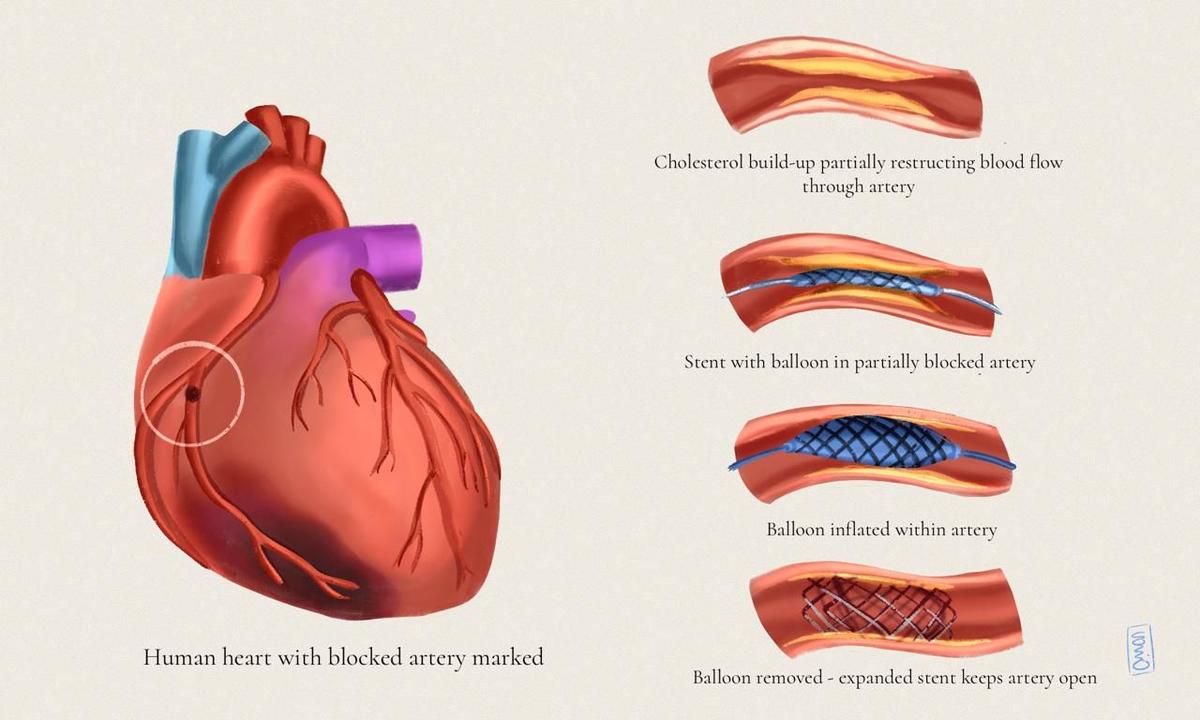
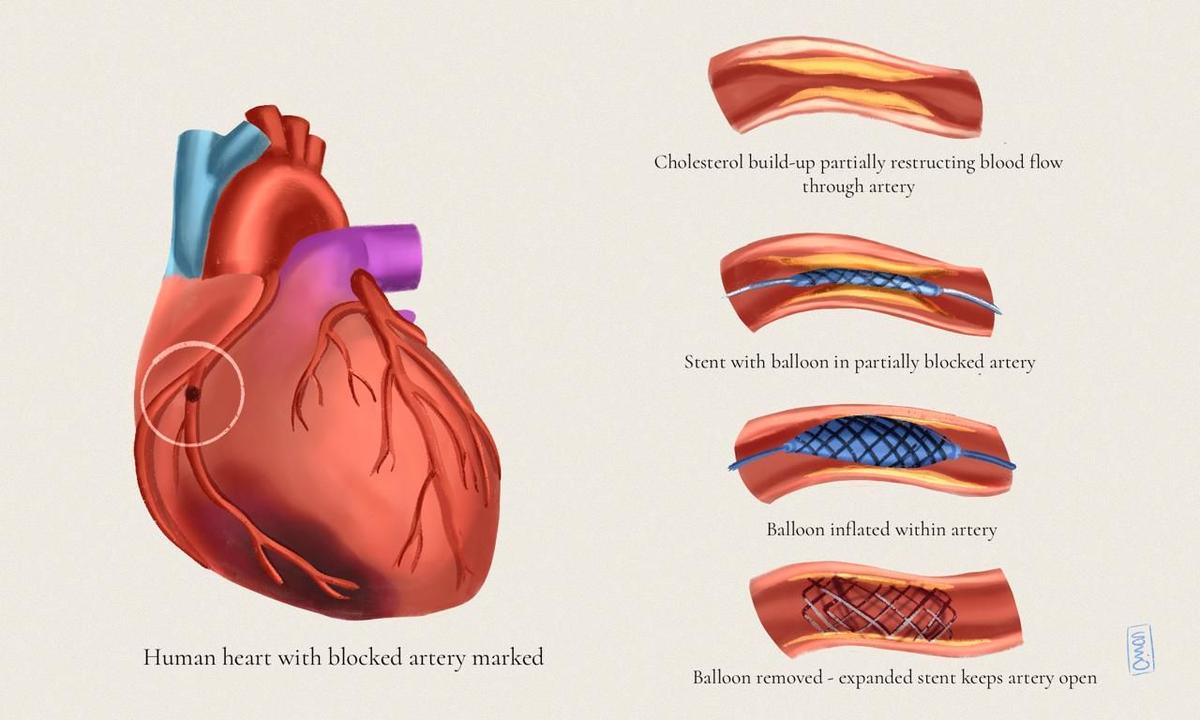
On reaching Vikasnagar’s Community Health Centre (CHC), 55 km away, they discovered no physician there. Finally, at round 3 pm, they discovered assist on the Swami Vivekanand Charitable Hospital in Dharamwala, about 70 km from their hometown. This is the place Jassuram lastly obtained an electrocardiogram (ECG) achieved, which indicated he had suffered a coronary heart assault. The medical doctors rushed him for an angiography, the place they discovered he had a 100% blockage in one in every of his coronary heart vessels. They carried out an angioplasty the place a balloon was despatched to the blocked coronary heart blood vessel to widen it, and a mesh tube known as a stent was positioned there. The time taken from his first signs at 10:30 am to his first ECG was 4.5 hours, and it might be one other 40 minutes earlier than he the angioplasty process was achieved.
The excellent time that guidelines advocate for a affected person with a coronary heart assault to get an ECG and have it interpreted is 10 minutes of contact with a medical group.
Jassuram’s lengthy journey for an ECG is typical of what sufferers in rural areas face.
Dr. Gayatri, illustrator, Nivarana
While poor entry to healthcare in rural India is a well known reality, does residing in a metropolis assure well timed care? In December 2025, Usha Amin, a retired instructor, felt breathless for 2 consecutive days on her morning stroll; she discovered her pulse to be 33 on her digital BP machine (regular pulse being 60-80beats/min). Alarmed, she known as her son and rushed to the closest multispecialty hospital in Thane, which falls within the Mumbai Metropolitan Region.
An ECG confirmed Usha had developed a 3rd diploma coronary heart block, a severe situation the place {the electrical} alerts from the higher chambers of the center are utterly blocked from reaching the decrease chambers of the center that may result in cardiac arrest. However the physician on obligation knowledgeable them that the heart specialist was unavailable in the intervening time. Since Amin seemed secure, the household was informed that there was no want to fret, and she was suggested to schedule an appointment with the heart specialist and return the subsequent day. Amin’s daughter, an occupational therapist, realised the potential gravity of the extraordinarily low pulse charge and requested them to go to a different hospital’s emergency division, which appropriately identified her. They instantly admitted her and fitted her with a short lived pacemaker and scheduled her for surgical procedure to suit a everlasting pacemaker the subsequent day. “I feel extremely lucky that my mother did not face complications due to the delay, and we could refer her to another hospital,” her daughter Kritika Amin mentioned.
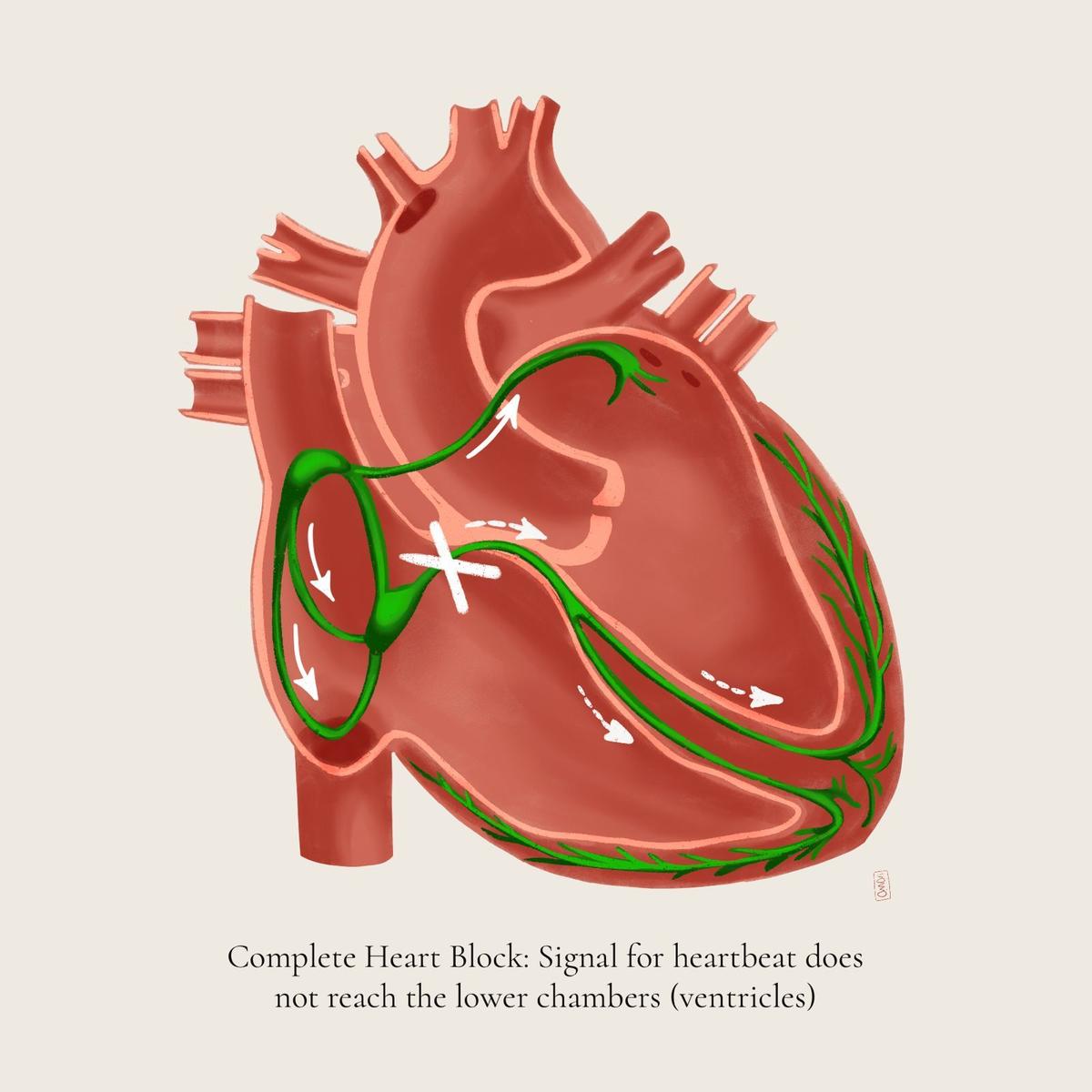
Dr. Gayatri, illustrator, Nivarana
Heart disease is the commonest reason for loss of life in India, accounting for 28.6 lakh deaths in accordance with the Global Burden of Disease, 2021. It is estimated that nearly 27% of all deaths in India are as a consequence of coronary heart disease, whereas 62% of all deaths as a consequence of cardiovascular disease (CVD) within the nation are untimely between the ages of 40 and 69 years. In 2014, the World Economic Forum and Harvard School of Public Health estimated India’s financial loss as a consequence of CVD between 2012 and 2030 to be roughly $2.17 trillion–about half of India’s 2025 GDP of $4.5 trillion. Yet, regardless of the speedy growth of medical amenities within the nation, there stays a lacuna on the subject of an acceptable and well timed response to emergency coronary heart circumstances. Here, we have a look at the varied gaps within the healthcare system that delay treatment for coronary heart disease and the price that we pay for it.
Most PHCs not geared up
The first step in diagnosing a coronary heart assault is present process an ECG take a look at, which data the center’s electrical exercise utilizing sticky patches known as electrodes, and provides out a report as a wave graph. This take a look at might help diagnose coronary heart assaults, irregular heartbeats (arrhythmias) and issues with blood stream. An ECG can detect a coronary heart assault as ST-segment elevation Myocardial Infarction (STEMI) circumstances — or non-STEMI inside minutes, and assist medical doctors plan additional treatment. However, even entry to this ECG is not frequent in India.
ECGs are at present accessible in district hospitals and neighborhood well being centres in India, that are tertiary healthcare centres. Most main well being centres (PHCs), that are the primary level of contact for sufferers in rural areas and are geared up with medical officers, wouldn’t have ECG machines. While the 2025 National Essential Diagnostic List recommends that ECG be accessible on the PHC degree, its implementation is anticipated to take time, time which tens of millions in India wouldn’t have.
Meanwhile the provision in greater centres is additionally not assured. “ECGs are not available in many of the CHCs here and patients have to travel all the way to the district hospital (2-3 hours away) to get an ECG done, ” mentioned a health care provider who works at a non-profit within the tribal district of Surguja in north Chhattisgarh.
Despite being comparatively cheap and straightforward to conduct, the provision of ECGs is restricted to large metros and hospitals in India, and there is a scarcity of skilled personnel to interpret the outcomes, says Yogendra Singh, director-interventional cardiology at Max Healthcare, Dehradun. “If a patient gets chest pain in Uttarkashi [in Uttarakhand], he has to travel at least 40-50 km to get an ECG done without which he cannot even be given an Ecospirin [a blood thinner]”, he says, emphasising the necessity to make ECGs accessible and accessible to individuals to detect coronary heart assaults early.
Doctors are usually not essential to be current to learn the ECGs, a number of research (here and here) have proven how tele-ECGs, carried out by frontline well being employees, might be electronically despatched to medical doctors and nurses for additional interpretation and recommendation, saving essential time and cash, in reaching greater centres.
Heart assault mortality
Indians undergo from coronary heart disease about 10 years earlier than the Western inhabitants, whereas our deaths as a consequence of coronary heart assaults is twice that of Sweden, whilst their sufferers are 15 years older, mentioned S. Ramakrishnan, senior heart specialist on the All India Institute of Medical Sciences (AIIMS), New Delhi.
While the typical age at first coronary heart assault in Western Europe, China, and Hong Kong is 63 years, it is 53 years in South Asia, and about 10% of our sufferers are under the age of 40 years. A number of factors, like hypertension, poor ldl cholesterol management, diabetes, sedentary existence, excessive belly fats, poor weight loss plan, in addition to genetic elements, play a job, together with life-style elements comparable to smoking and extended stress. Poverty additionally performs a job — poor individuals are extra prone to devour tobacco and alcohol and not devour fruits, greens, fish and fibre — and this will increase danger for coronary heart disease.
What’s worse is that most individuals have no idea that they’re in danger for coronary heart disease as a consequence of insufficient screening and poor consciousness. “In India, major heart attacks and death are often the first symptoms of heart disease,” mentioned Dr. Ramakrishnan. Despite having 315 million with hypertension and 101 million with diabetes in accordance with the Indian Council of Medical Research’s INDIAB study, there is low consciousness of blood stress and blood glucose, even amongst these with the disease, and 57% of the population doesn’t meet the WHO tips for bodily exercise.
Further, varied research have proven that sufferers with coronary heart disease in India have a higher proportion of STEMI circumstances. STEMI is a extra extreme sort of coronary heart assault brought on by the entire blockage of a coronary artery, proscribing blood to the key a part of the center and requiring pressing emergency care. The research additionally present that STEMI sufferers in India are prone to be poorer, present signs late, get inappropriate treatment and have a better probability of dying inside a month of the primary month.
While well timed treatment of STEMI circumstances in India will enhance the standard of life and additionally save lives, “the most common treatment an average Indian gets for a heart attack is no treatment,” says Dr. Ramakrishnan. Either sufferers don’t attain the hospital in time, or the hospitals they attain wouldn’t have the infrastructure or experience to deal with coronary heart assaults, he added. Late treatment will increase the danger of loss of life and problems, will increase probabilities of muscle injury and even when the affected person survives, she or he finally ends up having coronary heart failure, provides.
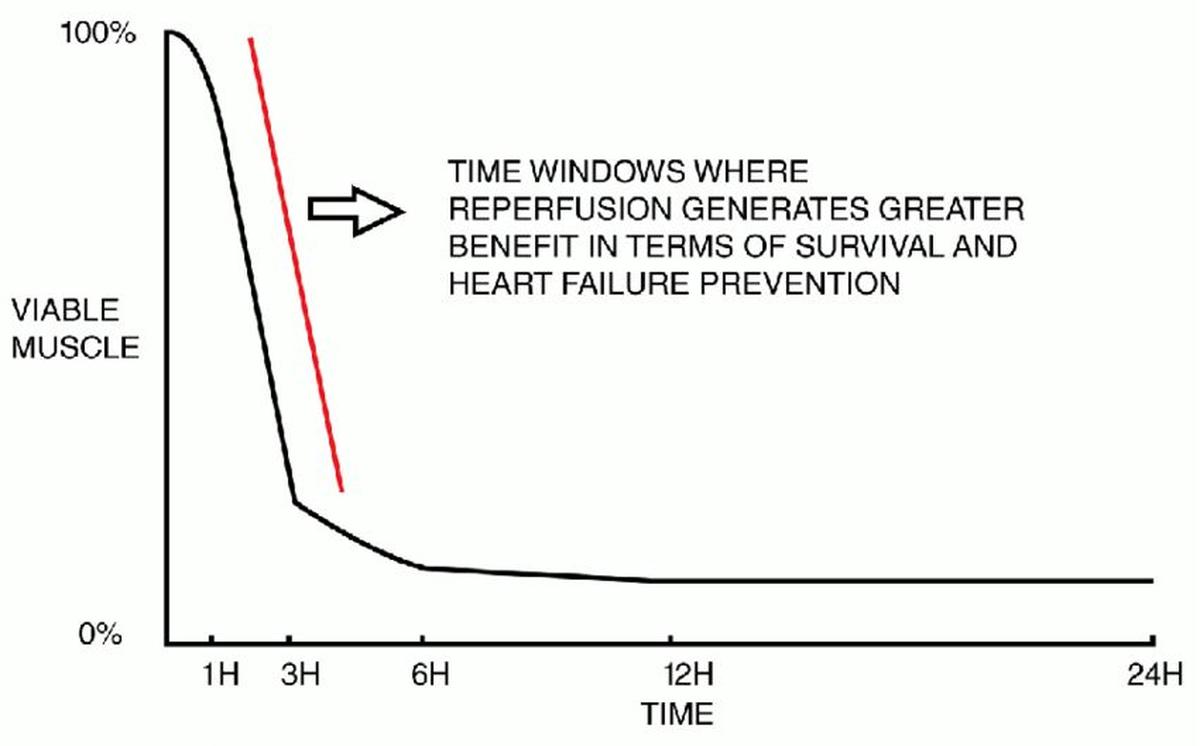
Source: https://doi.org/10.12688/f1000research.10553.1
| Photo Credit:
Source: https://doi.org/10.12688/f1000research.10553.1
‘Time is muscle’
When it involves the center, cardiologists typically like to make use of the phrase ‘time is muscle.’ Every minute of delay in getting treatment causes irreversible loss of life of the center muscle. Restoring blood provide to the center can cut back injury to the center, enhance survival charges and stop deaths.
In STEMI circumstances, for instance, the important thing treatment is reperfusion, which includes opening the blocked blood vessel. This might be achieved both by giving thrombolytic remedy, which is medication that bust the clots within the artery or by means of main percutaneous coronary intervention (PCI) or an angioplasty. While PCI is the gold normal of treatment, a really small share of Indian sufferers get PCI as treatment, and even getting thrombolytic remedy within the treatment window is not widespread. Various registry databases present that solely 5 to 10 in 100 sufferers bear well timed PCI whereas 36-60 out of 100 bear thrombolysis.
Another method of mixing the 2, is known as pharmaco-invasive remedy, the place thrombolytic medication are given to the affected person until the affected person might be transferred to a hospital with a cath lab. This has been efficiently carried out as a hub-and-spoke mannequin in lots of elements of the nation.
In different circumstances comparable to in conduction defects, cardiac muscle dies due to the irregular pumping of the center. Immediately addressing this through medication or a short lived pacemaker ensures that the injury to the center muscle is saved to a minimal.
In case of any emergency coronary heart situation, detecting and treating instantly is of paramount significance to make sure that as a lot of the center muscle as potential might be saved.
Treatment home windows
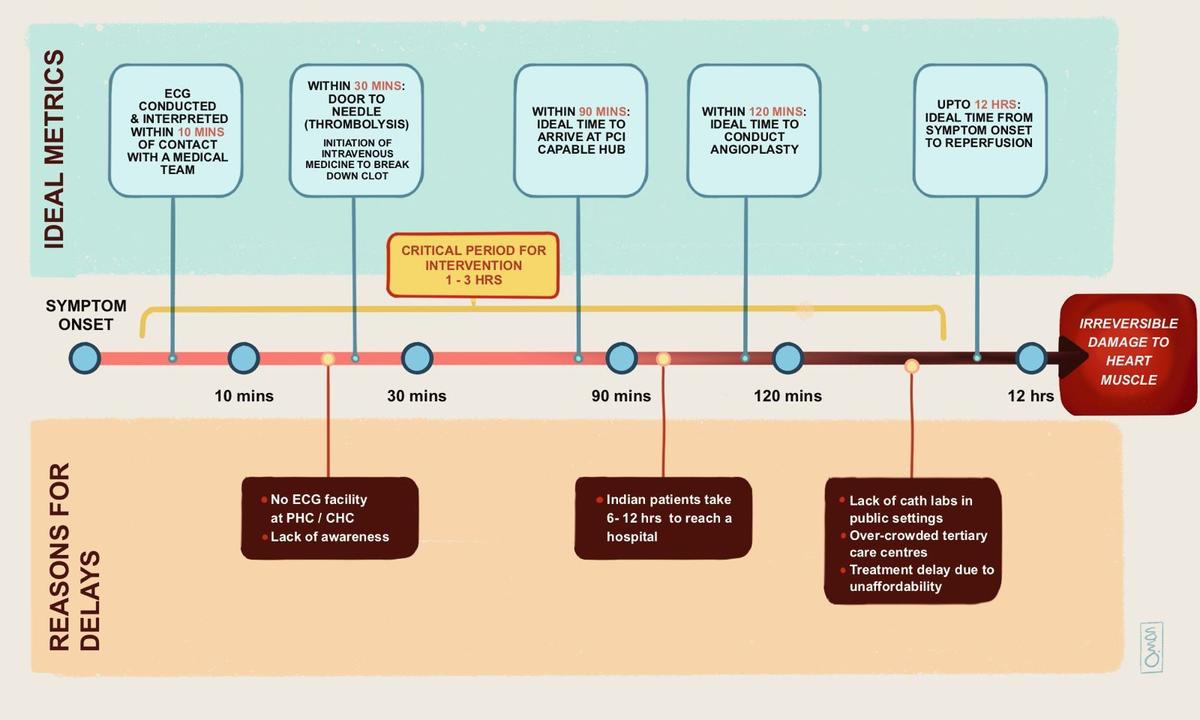
The most important time for intervention is between 1-3 hours of the center assault. The excellent time to conduct an angioplasty is inside 120 minutes or two hours of the primary medical contact. Treatment most helpful inside three hours of a coronary heart assault.
Jassuram and his son needed to waste 4 and half valuable hours travelling from one centre to a different earlier than getting the treatment that would save his life.Most Indian sufferers attain the hospital between 6 hours on common, and as much as 12 hours within the hilly States of India, in accordance with varied coronary heart registries, after struggling vital injury to their coronary heart muscular tissues. A study in Denmark has proven {that a} one hour delay in beginning treatment after the primary contact within the well being system results in a 15% enhance in deaths inside three-and-a-half years, whereas it is doubled if the delay is of three hours.
Treatment window within the Indian context
| Metric | Target time | Description | |
| Door-to-Needle (Thrombolysis) | ≤half-hour | From hospital arrival to beginning thrombolysis at spoke/non-PCI centres | |
| Door-to-Balloon (main PCI) | ≤90 minutes | Arrival at PCI-capable hub to balloon inflation | |
| First Medical Contact (FMC) to Reperfusion | ≤120 minutes | FMC to PCI or thrombolysis; ≤90 min most well-liked for direct PCI | |
| Symptom Onset to Reperfusion | Within 12 hours | Best <6 hours; pharmacoinvasive PCI 3-24 hours post-thrombolysis | |
| First Medical Contact-to-Needle (prehospital) | ≤120 minutes | Community-level purpose for thrombolysis initiation |
Source: Guidelines by Cardiological Society of India, American Heart Association, TN-STEMI mannequin, National STEMI tips
Why the delays
Lack of consciousness: A 2023 study, which audited civil-registered untimely (30–69 years) deaths as a consequence of acute cardiac occasions or strokes in Faridabad, Haryana, discovered that solely about 11% of the sufferers reached an acceptable well being facility inside one hour. About 4 in 10 of them didn’t attain the right facility as a consequence of a delay in recognising the symptom or its seriousness; 2 in 10 didn’t attain the right facility as a consequence of a delay in reaching the hospital — as a consequence of lack of transport, absence of an attendant or reaching a centre with out acceptable amenities — and lastly 1 in 10 as a consequence of unaffordability or lack of a specialist.
This was just like what was discovered by analysing the outcomes of the CREATE registry — a potential research of 20,937 acute coronary syndrome (ACS) sufferers throughout 89 Indian hospitals between 2001-2005 — poor consciousness of signs, logistical challenges in reaching the hospitals and well being system gaps have been key causes sufferers obtained delayed treatment.
“Sometimes there is ignorance, sometimes there is denial, [patients think] that it will get relieved with local treatment or an antacid,” says H. S. Isser, professor and head of cardiology, at Vardhman Mahavir Medical College and Safdarjung Hospital, Delhi. If the center assault is very extreme, the affected person might collapse and is instantly rushed to the closest hospital, but when the signs are delicate, like sweating, ache and breathlessness, sufferers typically strive dwelling treatments and watch for one or two hours earlier than reaching the hospital, he notes.
Lack of cath labs in public settings, over-crowded tertiary care centres: Even when sufferers attain hospitals, many hospitals are usually not geared up with ECG machines or the manpower to interpret them. Even if ECGs can be found, sufferers are sometimes referred to greater centres which have cardiologists and cath labs, the place angioplasties are carried out. There are about 2,500 cath labs within the nation, most of them within the metros of the developed States of Maharashtra, Kerala, Gujarat, Tamil Nadu and New Delhi.
Thrombolysis use is additionally restricted as a result of non-specialist medical doctors don’t need to danger giving clot-busting medication, which may have unwanted side effects like inside bleeding, with out the presence of cardiologists. There are about 6,500 cardiologists in India, lower than 0.45 per 100,000 inhabitants and most of them are concentrated in city cities.
Also, regardless of the growing variety of cath labs, 90% of them are within the non-public sector, and most States, particularly within the North and the East, need to make-do with having just one tertiary centre within the State capital with a cath lab– resulting in overcrowding and lengthy ready instances for sufferers.
Unaffordability: Even if the treatment is accessible and accessible, the query that bogs down most households is how costly it might be. Given the dearth of diagnostic amenities within the public sector and lengthy ready traces, most sufferers depend on non-public hospitals for hospitalisation of cardiac circumstances, however this has led to excessive out-of-pocket bills in sufferers. Nearly half of coronary heart sufferers expertise catastrophic health expenses — when the well being expense is better than 40% of the household’s annual revenue — as a consequence of hospitalisation, whereas 43% face it as a consequence of outpatient bills.
The Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (AB-PM JAY), India’s flagship medical health insurance scheme, has improved entry to coronary heart procedures that have been out of attain for common Indians — the speed of angioplasties rose by 61% and angiographies by 132% — after the launch of the scheme in Kashmir, notes a 2025 study. While this is a welcome change, there is an over-reliance on the non-public sector — 79% of all cardiac procedures below the scheme are carried out within the non-public sector. This has led to circumstances of malpractice on one hand and denial of the scheme on the opposite — hospitals in a number of States have protested nonpayment of dues and refused to supply treatment below PMJAY, leaving tens of millions with out protection.

57-year-old Raiz travelled 100 km to Delhi’s Govind Ballabh Pant Hospital as a result of he was informed PMJAY was not accessible in Jaypee Hospital in Bulandshahr
| Photo Credit:
Courtesy, Nivarana
Many sufferers we met outdoors Delhi’s public hospitals claimed to have been informed the scheme is not accessible within the non-public hospitals of their districts, which compelled them to hunt care in crowded public hospitals, even when they face delays. One affected person, 57-year-old Raiz, suffered a coronary heart assault on December 30 in Bulandshahr’s Shikarpur however got here all the way in which to Delhi authorities’s Govind Ballabh Pant Hospital 100 km away, as a result of the treatment would be freed from price. Raiz, a labourer, had first achieved preliminary assessments together with an ECG and 2D ECHO at Jaypee Hospital, Chitta, however refused additional treatment when he was informed that an angiography would price ₹30,000. While the hospital is empanelled below the PMJAY scheme for cardiology in accordance with PMJAY’s web site, Raiz says the hospital mentioned they don’t settle for Ayushman Bharat card sufferers and Raiz determined to attend. Like most Indian sufferers who set out on a journey, he tried to take care of all his unfinished enterprise first, which included getting one in every of his daughters married. A coronary heart assault that ought to have been attended to throughout the first two hours, would solely be handled a month later.
Sheespal Bhagel, head of medical operations at Jaypee Hospital says, “Our name has changed from Jaypee Hospital to Manush Jaypee Hospital on January 14, 2026 which has caused a change in the status on the [PMJAY] portal. We have sent applications to Lucknow so that the hospital, with its new name, is empanelled again.”
Dr. Gayatri, illustrator, Nivarana
After a coronary heart assault
Once an individual has a coronary heart assault, they need to take medicines for all times. There is, nevertheless, no mechanism to make sure sufferers have entry to reasonably priced medication within the public system. “Patients do not get their prescribed medicines in PHCs or CHCs but have to travel all the way to the district hospital to get them,” says the Chhattisgarh physician. Given the price, intermittent unavailability of medicines and the time concerned, most sufferers have to purchase the medication out-of-pocket from the non-public sector, he provides.
The scenario is not higher in Delhi’s tertiary care hospitals, which cater to sufferers throughout the State and different neighbouring states. Many of the sufferers we met on the cardiology OPD of Delhi’s tertiary care hospitals didn’t know whether or not they had suffered a coronary heart assault; that they had been going from hospital to hospital and not using a clear analysis or a plan. It took them weeks to get their reviews prepared and get an opportunity to see the physician whereas the ready time for procedures was in weeks or months.
At AIIMS Delhi, the ready interval for cardio-thoracic and vascular surgical procedure is as much as two years as a consequence of heavy affected person load, in accordance with a solution given in Parliament in July 2025, by Prataprao Jadhav, Union Minister of State within the Health Ministry. Just a number of metres away is one other authorities tertiary care hospital, Vardhman Mahavir Medical College and Safdarjung Hospital, with a totally geared up 12 bedded ‘Heart Command Centre’ that is making an attempt to cut back delays in treatment for coronary heart sufferers. While the sufferers on the whole emergency sufferers might undergo delays in getting recognized and referred for angioplasty, they get shortly triaged and obtain thrombolysis and angioplasty right here. The centre boasts of 4 cath labs with two being accessible 24/7.
“This is a rare kind of set-up in the public setup; we do 20 angioplasties daily out of which 5-10 are heart attack patients receiving emergency angioplasties,” mentioned Dr. Isser. The hospital, which will get sufferers from Delhi and different North Indian states, has a capability of 110 beds for cardiac sufferers however typically faces a scarcity, he says.
What if coronary heart sufferers didn’t need to journey lengthy distances to different cities and have been handled close to their properties? That is a query ready to be answered.
(Swagata Yadavar is an impartial journalist. swagatayadavar@gmail.com)
(This is the primary a part of a three-part collection on the well being system’s response to coronary heart assaults. This collection is a challenge of Nivarana, a digital public well being platform and has been supported by Sunfox Technologies)